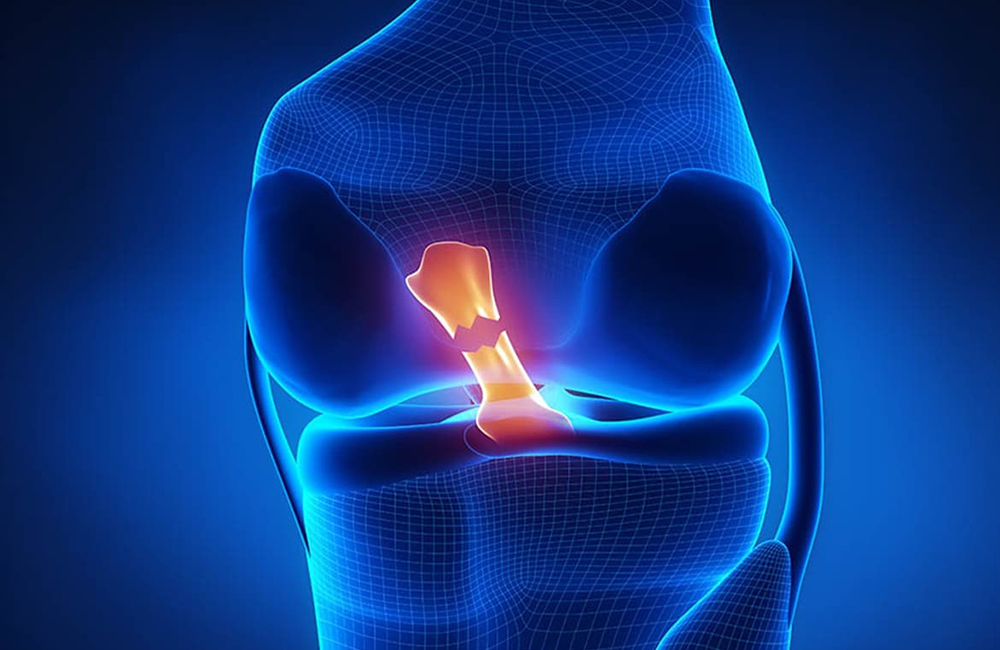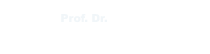
Hip avascular necrosis, commonly known as “hip bone collapse,” is a serious condition that threatens the hip joint, particularly in young and middle-aged patients. Medically referred to as femoral head avascular necrosis, it occurs when the blood supply to the femoral head is disrupted, leading to the death of bone tissue.
If not diagnosed early, collapse of the femoral head may develop, and the condition can progress to the need for total hip replacement.
In this article, we will discuss treatment options for hip avascular necrosis, focusing particularly on the Bioplasty method, which has gained increasing attention in recent years, and its advantages compared to other treatments.
What Is Hip Avascular Necrosis?
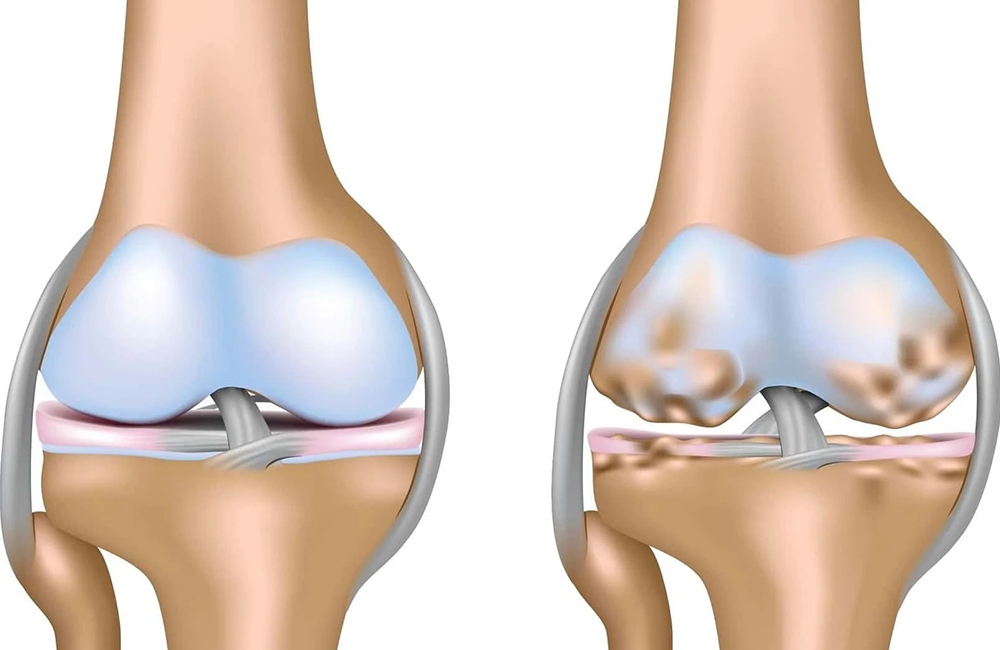
The femoral head forms the spherical part of the hip joint. When its blood supply is impaired, bone tissue begins to lose vitality.
Initially, there may only be bone marrow edema and microdamage. However, as the disease progresses, structural collapse of the femoral head and joint surface deterioration may occur.
Common Causes:
- Long-term corticosteroid use
- Alcohol consumption
- Trauma
- Blood disorders
- Idiopathic (unknown cause)
In early stages, pain is typically felt in the groin area. As the condition progresses, limitation of movement develops.
Treatment Options for Hip Avascular Necrosis
Treatment is planned according to the stage of the disease. The most commonly used approaches include:
- Conservative treatment (rest, reduced weight-bearing)
- Core decompression
- Bioplasty
- Vascularized bone graft
- Total hip replacement
In early stages, the primary goal is to preserve the femoral head and prevent collapse.
What Is Bioplasty?
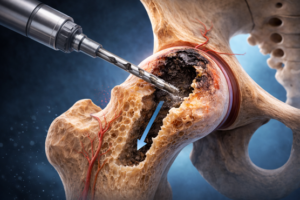
Bioplasty is an advanced version of the traditional core decompression procedure, enhanced with biological support.
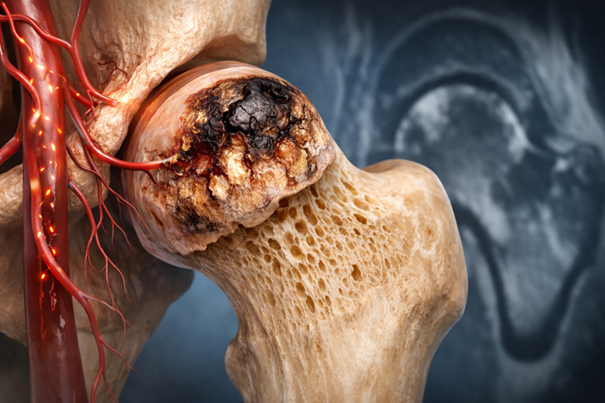
In this procedure:
- A small channel is created toward the femoral head
- The necrotic area is removed
- Biological materials that promote healing (bone graft, biological matrix, bone marrow aspirate concentrate, etc.) are applied
The goal is not only to reduce pressure but also to stimulate bone regeneration.
The core philosophy of Bioplasty is:
“Not just decompression, but active biological repair.”
Success Rate of Bioplasty
Scientific studies indicate that in early-stage (Ficat stage I–II) hip avascular necrosis, Bioplasty shows a success rate between 70–85%.
Success criteria include:
- Pain reduction
- Prevention of femoral head collapse
- Delay of hip replacement
In active patients under 50 years old, delaying hip replacement for many years represents a significant advantage.
Why Is Bioplasty Superior to Core Decompression?
Traditional core decompression primarily reduces intraosseous pressure but does not actively stimulate biological healing.
Advantages of Bioplasty:
️1. Promotes Biological Repair
Bone marrow cells and graft materials support new bone formation.
️2. Reduces Collapse Risk
Filling the necrotic area provides structural mechanical support.
3. Higher Success Rate
Clinical outcomes reported in the literature are superior to decompression alone.
4. Delays the Need for Hip Replacement
Especially beneficial in younger patients.
Who Is a Candidate for Bioplasty?
- Patients with early-stage hip avascular necrosis
- No femoral head collapse yet
- Young and active individuals
- Patients wishing to delay hip replacement
In advanced stages (with collapse), total hip replacement becomes the more appropriate option.
Comparison: Bioplasty vs Core Decompression
| Criteria | Core Decompression | Bioplasty |
| Main Goal | Reduce intraosseous pressure | Remove necrotic bone + biological regeneration |
| Biological Support | No | Yes |
| Mechanical Support | No | Yes |
| Success Rate (Stage I–II) | 55–70% | 70–85% |
| Delay of Hip Replacement | Limited | More significant |
| Revision Need | More frequent | Less frequent |
Comparison with Total Hip Replacement
Total hip replacement is the most effective treatment in advanced-stage disease.
However:
- Prosthesis lifespan averages 15–20 years
- Revision surgery risk is higher in young patients
- It is a major and irreversible surgery
Therefore, hip-preserving procedures are preferred in younger individuals whenever possible.
Bioplasty acts as an important “bridge treatment.”
Surgical Process and Recovery
Bioplasty:
- Is performed through a small incision
- Requires short hospitalization
- Allows early mobilization
Weight-bearing restriction is recommended for 4–6 weeks.
Complete biological healing may take several months.
Are There Risks?
As with any surgical procedure, risks include:
- Infection
- Insufficient healing
- Progression to collapse
- Eventual need for hip replacement
However, with proper patient selection, success rates are high.
Why Is Early Diagnosis Important?
MRI is the most sensitive method for detecting femoral head avascular necrosis in early stages.
Early diagnosis allows:
- Prevention of disease progression
- Reduced likelihood of prosthesis
- Preservation of the native hip joint
Conclusion
Hip avascular necrosis is a condition that can be successfully managed when diagnosed early.
Bioplasty offers significant advantages over traditional core decompression by:
- Supporting biological healing
- Reducing collapse risk
- Delaying hip replacement
- Providing hip preservation in younger patients
The most appropriate treatment should be determined individually, considering disease stage, age, activity level, and bone quality.